IN THIS POST
Anemia in dogs, or a decrease in useful or functioning red blood cells, can be a serious cause for concern. It is often a severe condition in and of itself, and it may be a symptom of a large number of diseases and illnesses. This makes it important to figure out the right underlying problem before starting treatment. Learn more about some of the most common causes of anemia in dogs, and what you can do at home.
What is Anemia in Dogs?
Anemia is a general term used when there isn’t a sufficient number of functioning red blood cells in circulation in the bloodstream. Red blood cells are needed to carry oxygen and other nutrients to the various cells and tissues of the body. When there aren’t enough, the body struggles to provide enough nutrients and oxygen to keep cells alive. This leads to issues in other body systems. Typically, anemia is checked via a packed-cell-volume (PCV), also called a hematocrit, test that determines the percentage of red blood cells to other cells and nutrients in the blood. For dogs, a PCV between 35-45% is normal. Under 35% is anemia, while over 45% is called polycythemia.
Anemia can be regenerative or non-regenerative. With regenerative anemia, the bone marrow still responds to signals to produce more red blood cells. However, it just can’t keep up with demands. In nonregenerative anemia, the bone marrow either isn’t prompted to respond, or doesn’t respond adequately to replace red blood cells. Causes such as blood loss from injury, toxins, infections, and immune system disorders are usually regenerative. Issues such as nutritional deficiencies, chronic diseases, and cancers lead to non-regenerative anemias.
General Signs of Anemia in Dogs
General signs present in all types of anemia include excessive panting, a decrease in activity, and changes in behavior. Your dog may also eat or drink less or have changes in bowel and urinary habits. Some

dogs may not want to perform typical daily activities or get tired very quickly. In severe cases, your dog’s gums or tongue may turn pale.
For dogs with pale gums, a test can be done by gently pressing on the gums and then removing your finger. If color does not return to the pressed spot in 2-3 seconds, this is a sign of something wrong. Signs can come on gradually, usually with long-term disease, or rapidly with immune or injury-related illnesses.
Regenerative Anemia in Dogs
Auto-immune Mediated Anemia
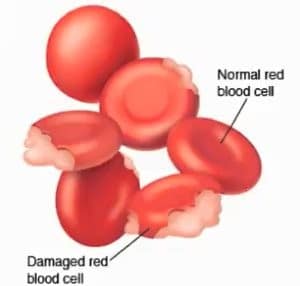
Auto-immune mediated anemia, also called auto-immune hemolytic anemia (IMHA) is an inflammatory immune reaction where the body begins to destroy its own red blood cells (hemolysis). Dogs with IMHA often present with symptoms suddenly, and may be jaundiced, have an enlarged spleen, or become feverish. IMHA can be determined with a few tests. These include PCV and other bloodwork, X-ray or ultrasound of the abdomen to check the spleen, and fecal exams to rule out parasites.
Treatment involves controlling the immune response to allow for red blood cell production. Other treatments include blood transfusions in severe cases, supportive care, and sometimes medications to help promote RBC (Red Blood Cell) production. Prevention of IMHA is hard, as symptoms often do not present until a dog is very ill. Because of the severity, and sudden onset, it can also be difficult to treat.
Toxic Ingestion
Ingestion of toxic items can also lead to anemia in dogs. Chemicals such as rat poisons prevent proper clotting of blood, and can also destroy blood cells, resulting in anemia. Over-the-counter medications commonly prescribed to humans, such as ibuprofen or aspirin, or foods such as onions can also cause a toxic response. Some plants and heavy metals such as lead can also cause toxic anemias.
Removal of and treatment of the toxicity is best for treating toxic-ingestion anemia. Supportive care such as hospital stays, IV fluids and medications, supplementation with erythropoietin to stimulate cell production, or blood transfusions may be needed to replace lost blood. Prevention is easier compared to other causes of anemia. Avoid letting your dog have access to medications or foods that can cause a toxic response. On walks, keeping your dog leashed and avoiding potentially harmful items such as strange plants or trash can prevent ingestion of these items.
Infections
Infections caused by bacteria or viruses can lead to anemia as the body struggles to fight it off. The infection can also attack places where blood cells are made, or directly attack the red blood cells themselves. Ehrlichia bacteria and Babesia organisms, both transmitted by ticks, are the most common that lead to anemia as a symptom of infection. Treatment includes both treatment of the infection itself through the use of antibiotics if caused by bacteria, as well as secondary symptom treatment and palliative care, such as IV fluids, nutritional support, and boosting RBC production.
Prevention of tick bites is best. This can be done through regular use of anti-tick medications, as well as keeping dogs out of heavily wooded and brushy areas where ticks live.
Injury and Blood Loss
Rapid loss of blood due to injury can cause acute anemia. Trauma, or injury, has many symptoms, most notably excessive bleeding from wounds, or internal bleeding from damaged or bruised organs. A dog with external injuries may limp or lick at wounds, while a dog with internal injuries may suddenly become lethargic, be painful or guard the abdomen, or become pale or blue in the tongue or gums. Diagnosis of injury involves a thorough physical exam for visible wounds, as well as checking internal organs through X-rays, ultrasound, and bloodwork as needed.
Treatment involves stopping the bleeding, including applying pressure to external wounds through the use of bandaging or hand-held pressure. Treatment of internal injuries can be more complicated. It can include supportive care while the body heals, removal of blood pooling in body cavities, or even removal of organs such as the spleen if affected. For more chronic bleeding disorders, such as ulcers, treatment of the ulcer with oral medications can help resolve the bleeding. Prevention of blood loss by treating minor injuries before they worsen, avoiding dangerous situations when possible, and veterinary exams if an internal injury is suspected can help.
Parasite Infections
In addition to tick-borne parasites, other parasites such as heartworm and intestinal worms can lead to anemia in dogs. Heartworm infections lead to blocked vessels which can prevent regular blood flow through the body. Intestinal parasites, like hookworms, can sap needed nutrients for producing red blood cells and also cause internal bleeding. Bloodwork, such as a heartworm snap test, or stool sample testing to look for parasite eggs can be done to determine if parasites are present.
Treatment can be tricky in severe heartworm cases. The parasites will need to be killed off gradually to prevent dead worms from clogging arteries and causing a heart attack or stroke. Often, low-dose anti-parasitics are given over a period of weeks to months with intense veterinary monitoring to watch for signs of distress.
An oral dewormer can be given to remove intestinal parasites. In severe cases, it should be given once or twice more over a period of a few months to ensure all parasites have been cleared. Prevention through the use of monthly heartworm tablets, annual intestinal deworming, and regular testing can prevent and catch infections before they become serious.
Non-Regenerative Anemia in Dogs
Poor Nutrition
Nutritional deficiencies are a rare cause of anemia in dogs, due to the widespread use of commercial dog foods that are nutritionally complete. The body requires several nutrients, including iron, several B vitamins, vitamin E, and copper in order to produce red blood cells. Other nutritional deficiencies, such as low phosphorus caused by chronic illness, can also result in anemia. Bloodwork to check for deficiencies, or to find other underlying causes such as chronic kidney disease, can help determine the cause of nutritional anemia.
In most cases, treating the underlying condition and supplementing the missing nutrients can reverse the anemia. Feeding a balanced diet can prevent food-based nutritional anemias. It is also important to monitor conditions where nutritional needs change rapidly. These include life changes such as pregnancy, lactation, or even extreme sporting or exercise.
Chronic Illness
In normal bodies, red blood cells are regularly produced, circulated, and then replaced as they are removed from the bloodstream. With some illnesses, the body may not be able to produce enough new red blood cells to replace lost ones. A hormone produced by the kidneys, called erythropoietin, is responsible for stimulating RBC production in the bone marrow. The body cannot create enough new red blood cells If not enough is made, causing anemia in dogs. Chronic, long-term illnesses, such as kidney disease or problems with bone marrow production can result in this type of anemia.
As with other anemias, bloodwork to determine the underlying cause, as well as ruling out other health issues can determine if a chronic illness is to blame. Treatment can involve treating the underlying illness or providing injections of erythropoietin to supplement what the kidneys can’t produce. Supplementing nutrients such as phosphorus and iron can also help. Prevention is more difficult, due to the cause of this anemia. However, catching kidney and other chronic disease early, and keeping it under control, can help.
Bone Marrow Production
Issues with the bone marrow itself can cause non-regenerative anemia (called aplastic anemia if all cell types are affected, and red blood cell aplasia if only RBCs are affected). The bone marrow is a set of specialized cells within bones responsible for creating many of the blood’s circulating cells, including red blood cells. When there is a problem with their production, either due to injury to the bone marrow itself with some cancers, or a problem with stimulating the bone marrow with kidney disease, not enough red blood cells are produced to replace those lost in circulation.
Diagnosis of bone marrow disorders involves checking for and ruling out other causes of anemia through bloodwork. A bone marrow biopsy can be done to check the status of the cells within the marrow If the bone marrow is suspected to be the cause. Treatment involves getting any secondary issues under control, such as kidney disease. Treating tumors or cancers through chemotherapy or referral to an oncologist can also help. Medications such as erythropoietin can help stimulate bone marrow red blood cell production if the body can’t produce enough of its own.
Tumors
Tumors of the organs, such as hemangiosarcoma, cancers of the blood such as leukemia, ulcerated bleeding tumors, and other forms of cancer and growths can all cause anemia. This can be because the tumor changes the body’s ability to produce red blood cells if located in the bone marrow, actively destroys cells, uses up nutrient resources, or leads to chronic blood loss over time.
Diagnosis is tricky, and involves a full-body examination. Other tests, such as bloodwork to check overall organ function and PCV, and ultrasound or X-ray to check for masses in the abdomen, on the spleen, or in the lungs can determine if a tumor is present. Sometimes, a dog may be referred to an oncology specialist if the tumor is advanced or rare.
Treatment depends on the underlying cause. Removal of affected organs, such as the spleen, or the tumor itself may alleviate symptoms. In cases where the tumor has spread (metastasis) or is in an area where surgery isn’t an option, chemotherapies and other medical treatments can help to reduce or stop growth. Palliative care is another option. Pain medications, treating secondary infections, and keeping your dog comfortable can help, though it may not treat the underlying cause. Prevention is harder. Tumors can often be related to genetics or grow rapidly, leading to sudden, often surprising, onset of symptoms.
Anemia is a serious and sometimes difficult issue. There are many other potential, but less common causes of anemia. These include blood clotting disorders, genetic illnesses, and hormonal changes that have similar symptoms and treatments. With regular visits and care, you and your vet can better help ensure your dog stays happy and healthy.