IN THIS POST
Pale gums in dogs, along with lethargy are signs of a condition called anemia. Dogs normally have a medium to dark pink gum color; gently picking up the upper lip along the side of your dog’s muzzle near his canine teeth allows you to get a good look at your dog’s gums. Pale gums are more difficult to ascertain in breeds with pigmented gums. Other places that can be checked include the inner lip, the conjunctiva (inner eyelids), just inside the prepuce (skin covering the penis) or the vulva. Other signs of anemia include labored breathing, loss of appetite, increased heart rate, or signs of blood loss (bloody nose or blood in stool, urine, or vomit). This article covers the definition of anemia, its diagnosis, the more common possible causes, and treatment.
** If you notice a sudden onset of pale gums and weakness, especially with difficulty breathing and increased heart rate, please see your veterinarian immediately – this is a medical emergency and you could save your dog’s life. **
Pale gums in dogs
What are red blood cells?
Red blood cells, also known as erythrocytes, are the most numerous blood cells present in the bloodstream. They don’t have many of the structures such as a nucleus and mitochondria like other cells do, but instead are packed to the gills with hemoglobin molecules. Hemoglobin is a protein that carries oxygen from the lungs to all the other cells in the body. Red blood cells are produced in the bone marrow and are then released into the bloodstream. Once in the bloodstream, they carry oxygen throughout the body for about three months. As the red blood cells age or are damaged, the immune system removes them from the bloodstream. The immune system then breaks down the red blood cells and the components are used by the bone marrow to produce new red blood cells.
What is anemia?
Anemia is defined as a reduced number of red blood cells circulating in the bloodstream, a reduced amount of hemoglobin, or a combination of both. Anemia in and of itself is not a disease, but instead a symptom of an underlying illness. Anemia may be classified as regenerative or non-regenerative. Regenerative anemia means that lost or damaged red blood cells are being replaced by the bone marrow (though perhaps not as quickly as they are being lost or destroyed). Non-regenerative anemia means the bone marrow is not producing red blood cells above and beyond their normal capacity (or not even producing their usual number) and are therefore not replacing lost or damaged red blood cells.
Since red blood cells carry hemoglobin and hemoglobin carries oxygen throughout the body, a lower than normal amount of either red blood cells or hemoglobin can have grave consequences. Without sufficient oxygen to various organs, the organs sustain damage and eventually fail.
How is anemia diagnosed?
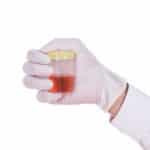
Anemia can be diagnosed with a simple blood test called a CBC, or complete blood count. Most veterinary hospitals have the capability to run a CBC in house. The CBC will measure the number of red blood cells and hemoglobin in the blood sample (as well as count the number of platelets and numbers and types of white blood cells). A similar test known as a PCV (packed cell volume) or hematocrit is often performed in conjunction with the CBC to verify the concentration of red blood cells. The blood sample is spun down in a centrifuge tube – the red blood cells will move to the bottom of the tube, the white blood cells in the middle, and the liquid (plasma) part of the blood will be at the top. The percentage of the tube that the red blood cells occupy is then measured. The PCV should be between 35-55%; anything below that is considered anemic for most breeds.
Another part of the CBC is a measurement of whether the anemia is regenerative or not. When an anemia is regenerative, the bone marrow releases immature red blood cells called reticulocytes in an attempt to bolster the amount of red blood cells in the blood quickly. The machine that runs the CBC is able to distinguish the reticulocytes from normal red blood cells, or a blood smear can be stained and examined under the microscope to look for reticulocytes.
What can cause anemia?
There are a number of conditions that can cause anemia; they can be broadly divided into three categories:
-
Conditions or diseases that cause blood loss
-
Diseases that cause red blood cell breakdown or destruction (hemolysis)
-
Diseases that decrease or suppress bone marrow production of red blood cells
Conditions or diseases that cause blood loss, leading to pale gums in dogs
Trauma
Usually the most obvious cause of blood loss is trauma, such as being hit by a car. Treatment consists of identifying the source of the blood loss and and to stop the bleeding. If the blood loss is severe, one or more blood transfusions will be recommended in order to support the organs while the active bleeding is stopped. Prognosis will depend on the extent of the injuries and the degree of blood loss. Loss of 30-40% of a dog’s blood volume without prompt replacement of the blood with IV fluids or blood transfusions will result in shock and likely death.
Parasites
Parasites such as hookworms and fleas survive by feeding on the blood of their hosts. Hookworms live in the small intestine and clamp their hooked head into the lining of the small intestine where they will feed for a few days before moving on to another site in the small intestine. Their previous site will continue to bleed after they move, and so with large numbers of hookworms and a small dog or puppy, the amount of blood loss can be quite severe. Similarly, fleas feed off the blood of dogs, and while this isn’t a problem for larger or adult dogs, a severe infestation of a small dog or puppy can induce anemia. With both hookworms and fleas, with a small enough puppy and a severe enough infestation, death due to severe anemia is a possibility.
Fleas are diagnosed by examination of the dog’s skin – with a severe infestation, it’s easy to see the fleas jumping and moving around in the fur. The presence of flea dirt, the blood-filled droppings of fleas, is also diagnostic. Hookworms are diagnosed with a fecal examination – examining the fecal sample under a microscope and looking for the characteristic hookworm eggs.
Treatment of fleas consists of using a fast-kill oral drug such as [Capstar], which kills fleas as soon as 30 minutes after administration. Continued treatment involves using a monthly flea and tick preventative such as the Seresto collar, Vectra 3D, Frontline Plus, or NexGard. Treatment of hookworms involves oral administration of a dewormer such as Panacur or Drontal Plus. In severe cases of parasite infestation, hospitalization with intravenous fluids, heat support, and blood transfusions may be recommended.
Tumors
Anemia can be caused by tumors (either benign or malignant) that begin to bleed into the abdominal cavity. The most common cause of sudden onset of anemia and weakness is a tumor of the spleen called a hemangiosarcoma, though the liver and heart are two other places where hemangiosarcomas can be found since they are cancers of the blood vessels. When hemangiosarcomas start bleeding, they basically rupture, dumping a large amount of blood into the abdomen, or in the case of a heart-based mass, into the pericardium, a sac of tissue that surrounds the heart. Other types of abdominal tumors may rupture, but they tend to bleed more slowly in comparison to the hemangiosarcomas.
Diagnosis involves collecting and analyzing the fluid in the abdomen, abdominal radiographs and/or ultrasonography. If surgery to remove the mass and stop the bleeding is being considered, chest radiographs may be a recommendation in order to determine if the lungs are clear of any cancer that may have metastasized.
Recommended treatment for ruptured tumors is emergency surgery to remove the tumor, or as much of it as possible, and stop the bleeding. However, hemangiosarcomas generally carry a poor prognosis. The median survival time with just surgery is three weeks to three months. With doxorubicin chemotherapy in addition to surgical removal of a splenic hemangiosarcoma, median survival time increases to four to six months. The prognosis for a heart-based hemangiosarcoma is very poor. The tumor bleeds into the pericardium, placing pressure on the heart, making it difficult for the heart to continue to beat and move blood throughout the body. The most successful treatment to date is to take the dog to a specialty center for a rather invasive surgery to have the pericardial sac removed, followed by chemotherapy. The average life expectancy for this course of treatment in about six months. Given the expense of the treatment and the relatively short survival time, it is not wrong to consider humane euthanasia in these cases.
Rodenticides (Mouse/rat poisons)
Some poisons used against rats or mice contain anticoagulants such as warfarin, brodifacoum, or bromadiolone. These anticoagulants inhibit an enzyme that reactivates vitamin K for continued use in the blood clotting cascade. As a result, after all the vitamin K in the body has been used up, appropriate blood clots can no longer form, and blood starts to leak out of the blood vessels, causing anemia and eventual death.
Signs usually appear 3-5 days after ingestion of the poison (after all the available vitamin K in the body has been used up) and include respiratory distress, coughing (including coughing up blood), lethargy, and loss of appetite. Some patients will develop pinpoint bruising, while those who are severely poisoned will bleed into the chest, abdomen, and possibly even into the brain and spinal cord.
If the ingestion of the poison is observed, inducing vomiting within the first four hours will help limit the toxicity. Oral administration of activated charcoal is next; this will help absorb the toxin and keep it from entering the bloodstream. If a large amount of poison was ingested, or if clinical signs have started, vitamin K1 therapy is begun. The amount of K1 needed is available in prescription strength only; over the counter supplements are not sufficient for treatment. Vitamin K1 supplementation will need to continue for two to four weeks, or until a clotting time test called prothrombin time (PT) comes back normal.
Diseases that cause hemolysis
IMHA
There are a couple of autoimmune diseases that cause the destruction of red blood cells, but immune-mediated hemolytic anemia (IMHA) is by far the most common. This disease may occur spontaneously, or may be a result of cancer (hemangiosarcoma, leukemia, lymphoma), infections (bacterial or parasitic), certain drugs (penicillins, sulfa drugs, cephalosporins, methimazole), or toxin (bee sting envenomation). In IMHA, the immune system stops recognizing the dog’s red blood cells as belonging to the dog and begins to attack the dog’s red blood cells. Many times, the underlying cause is unable to be identified, and this is known as primary or idiopathic IMHA. Breeds that are predisposed to developing primary IMHA include American cocker spaniels, Old English sheepdogs, Irish setters, poodles, and dachshunds.
In addition to pale gums and fatigue, weakness, or collapse, symptoms of IMHA can include shallow, rapid, or labored breathing, yellow discoloration of the eyes and skin (jaundice), darkened urine (orange or dark red), and reduced appetite. Diagnosis of the disease includes blood tests such as a CBC to measure blood cell and platelet counts, a chemistry panel and urinalysis to measure liver and kidney function, and a saline slide agglutination test or Coomb’s test to assess the immune system. Diagnostic tests may also include radiographs of the chest and either radiographs or ultrasound of the abdomen to screen for cancer.
Treatment of IMHA starts with suppression and modulation of the immune system, usually with a steroid called prednisone. Other immunosuppressive drugs are usually added to the treatment regimen, and consultation with a board-certified internal medicine or critical care specialist is usually recommended to come up with the best treatment plan based on your dog’s specific clinical presentation. Any underlying infections must be treated quickly and appropriately while the immune system is being suppressed, otherwise the infection can spread rapidly and overwhelm the body. Blood transfusions may be necessary during the initial phase of treatment in order to correct any anemia and make certain that your dog has enough red blood cells to continue to carry oxygen to his organs. A common complication of this disease is the formation of abnormal blood clots, so your dog may also be placed on medications such as low-dose aspirin therapy, Plavix, or heparin in order to help prevent clot formation and strokes.
Unfortunately, documented death rates for IMHA are rather high (29-70%) and relapse of the disease is rather common (12-24%). Most of the deaths occur within the first two weeks of diagnosis, but dogs that make it past that point have a six month survival rate of about 93%.
Bloodborne parasites
Of the bloodborne parasites that infect and destroy red blood cells, Babesia is the most common. Babesia are protozoans (single-celled organisms with a nucleus) that are transmitted by ticks, and are most commonly found in the southern United States. Greyhounds and pit bull terriers are particularly at risk.
Babesia infections, called babesiosis, can cause a range of symptoms and clinical signs. There may be a mild illness that passes quickly, or a full-blown sudden collapse with shock that rapidly leads to death. Some cases cause a chronic disease with severe and progressive anemia as the main symptom. Most dogs with babesiosis present to the hospital with the severe form of the disease; its symptoms include abnormally dark urine, pale mucous membranes, weakness, fever, swollen lymph nodes, and an enlarged spleen.
Diagnosis of babesiosis can be done by performing a blood smear and looking for the parasites inside the red blood cells using a microscope. Other blood tests are now available such as PCR and ELISA – these look for proteins produced by the Babesia organisms, but take a few days to get the results since they must be performed by an outside laboratory.
The approved treatment for babesiosis is an injection called imidocarb dipropionate. Clindamycin, an antibiotic, is used to treat humans with babesiosis, and while not specifically approved for use in dogs with babesiosis, it is a treatment option. Supportive care in-hospital with blood transfusions may also be necessary. Prognosis may be guarded depending on the severity of the symptoms at presentation. If the dog recovers, he will likely have a subclinical infection that may flare up in the future.
Toxins
Toxins such as zinc (pennies), onions, and garlic cause a hemolytic anemia. If the ingestion was recent (within the previous two hours), it may be possible to limit the toxicity by inducing vomiting (as long as there are no contraindications to vomiting). With onions or garlic, induction of vomiting is followed by oral administration of activated charcoal in order to prevent the toxin from leaving the gastrointestinal tract. If ingested pennies are unable to be removed via vomiting, then it may be possible to remove them using an endoscope. If not, then surgical removal of the pennies from the GI tract is indicated in order to prevent further intoxication from the zinc as the pennies continue to break down in the GI tract.
Hospitalization and careful monitoring of the patient’s CBC and chemistry panels are the next treatment. Intravenous fluids, supplemental oxygen, and blood transfusions may all be necessary depending on the severity of the toxicity. Early and aggressive intervention and therapy are key to surviving these toxicities.
Diseases that suppress bone marrow function
Chronic disease
Any severe or chronic disease such as kidney or liver disease, hyperadrenocorticism (Cushing’s syndrome) or hypothyroidism, can cause suppression of bone marrow function. This is the most common cause of anemia seen in dogs. Through various mechanisms in this nonregenerative type of anemia, red blood cell lifespan is shortened, metabolism of iron is inhibited, and the bone marrow’s response to signaling for more red blood cells is impaired. Treatment of the underlying condition leads to correction of the anemia.
Aplastic anemia
Aplastic anemia occurs when the stem cells in the bone marrow are replaced by fat cells. This type of anemia affects red blood cells, white blood cells, and platelets. The cause of aplastic anemia is often unknown, but some cases have been reported to occur in response to infections (parvovirus, Ehrlichia), drug therapy (chemotherapy agents, chloramphenicol, methimazole, fenbendazole, or whole body radiation. There may also be an autoimmune component to this anemia.
Diagnosis is made by bone marrow biopsy. Treatment consists of eliminating the underlying cause, if known, and providing supportive therapy in the form of antibiotics, transfusions, and possibly immunosuppressants such as prednisone or cyclosporine while the bone marrow recovers. In cases where the underlying cause is unknown (idiopathic), bone marrow transplantation may be beneficial, but this treatment is limited in availability and is still experimental.
Leukemia
Leukemia is cancer stem cells in the bone marrow. While rare overall, two forms are common in dogs: acute lymphoblastic leukemia (ALL) and chronic lymphoblastic leukemia (CLL). The acute form is more likely to produce an anemia because the bone marrow almost exclusively produces lymphocytes, a type of white blood cell, to the detriment of red blood cell production.
Clinical signs of leukemia include weakness, anorexia, vomiting, diarrhea, and sometimes bone pain. A diagnosis of leukemia is made using a blood test called a CBC. Another test called flow cytometry, which analyzes blood cells and looks for specific protein markers indicative of disease, may be helpful in making a final diagnosis of the specific type of leukemia.
Treatment of ALL must be aggressive, and a chemotherapy protocol called CHOP is the recommended therapy. CHOP consists of the chemotherapeutic agents vincristine, Cytoxan, and doxorubicin, and the steroid prednisone. A different chemotherapeutic agent is given every week, usually at an oncology practice (though some general practices are set up to be able to administer chemotherapy), while the prednisone is given at home. The entire protocol is 25 weeks in length, though very few dogs with ALL survive to finish the course of treatment. However, dogs will typically respond well and quickly to the chemotherapy before the disease becomes resistant to it.
The take-away message for pale gums in dogs
There are a number of reasons anemia can occur, including bleeding, destruction of the red blood cells, or suppression of the bone marrow that produces red blood cells. Determining your dog is anemic is relatively easy through the use of a complete blood count (CBC), but often, determining the exact cause of the anemia can be challenging. Consultation with a veterinarian specializing in internal medicine is often helpful if the cause of the anemia is not immediately obvious. However, all cases of anemia should be investigated with the help of your veterinarian so your dog can return to an active and healthy life.