IN THIS POST
- What is rabies?
- How is the rabies virus transmitted?
- Symptoms of rabies
- Treatment
- Prevention
- What does a vaccine do?
- What are the benefits of vaccination?
- What are some of the concerns of vaccination?
- How are adverse reactions handled?
- Are we over-vaccinating for rabies?
- Take-away message about the rabies vaccine
Rabies is a universally fatal disease that can be prevented with the rabies vaccine. This article discusses rabies, symptoms, treatment, prevention, and why the vaccine is so important. It also discusses some of the risks and concerns about the rabies vaccine.
What is rabies?
Rabies is a preventable viral disease that infects the central nervous system of mammals (including humans), eventually reaching the brain and causing death. Once a dog has been infected, the virus spends a few days attached to local muscle cells before penetrating local nerves and beginning its slow ascent to the brain. Once the virus is in the nervous system, it moves beyond the reach of the immune system.
The incubation period (time from infection to showing symptoms) ranges from one week to one year, depending on the distance the virus must travel to the brain, but in most cases, the incubation period in dogs is 21-80 days. Symptoms begin 2-3 days after the virus has reached the brain; it is at that point the virus shows up in the saliva and the disease becomes transmissible. Once even mild symptoms begin to show, death occurs within 10 days.
How is the rabies virus transmitted?
Once symptoms start, the virus is present in the infected animal’s saliva. The virus is then transmitted through the bite or deep scratch of a rabid animal in the vast majority of cases. The virus can also be transmitted through the saliva of a rabid animal coming into contact with open wounds or the mucous membranes of the victim. Worldwide, contact with a rabid dog accounts for 99% of all human cases of rabies; approximately 60,000 people are infected with rabies and die each year.
In the United States, prior to the introduction of rabies vaccine requirements in 1947, at least 6,900 dogs were laboratory-confirmed to have rabies each year. By the late 1960’s, that number had dropped to about 500 rabid dogs per year, and by 1980, the number had dropped again to fewer than 100 rabid dogs per year. In 2004, the canine rabies virus variant was considered to have been eliminated from the United States. However, 60-70 dogs in the United States are still reported to be rabid each year due to exposure to wildlife, especially bats, raccoons, skunks, and foxes; almost all the dogs were unvaccinated. Similarly in people living in the United States, most cases are due to wildlife exposure, but some United States residents contract rabies from exposure to rabid dogs while traveling abroad. In the United States, only 1-3 people are affected by rabies each year.
Symptoms of rabies
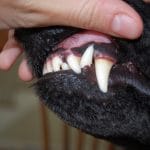
In dogs, there are three stages of symptoms. In the prodromal stage, which is the first 2-3 days after symptoms have started, the dog’s personality changes. The larynx begins to spasm and a voice change may be noted. The second stage is the excitative stage, which occurs over the next 1-7 days, and is the classic “mad dog” stage. Dogs have no fear and also suffer from hallucinations. If confined, the dog often attacks the bars of his cage. However, most dogs skip this phase and enter the paralytic stage, which occurs over the next 2-4 days. Weakness and paralysis set in. The larynx becomes paralyzed, which means the dog is unable to swallow, and therefore he drools and “foams at the mouth”. Death occurs when the virus paralyzes the muscles that control breathing.
Treatment
As soon as possible after an exposure to a potentially rabid animal, post-exposure prophylaxis must begin. In dogs with a current rabies vaccination, any wounds are thoroughly cleaned and another rabies vaccine is administered in order to boost the immune system and make certain the virus never reaches the nervous system. The Center for Disease Control (CDC) recommends 45 days of observation after the exposure. Similarly, for dogs that don’t have a current rabies vaccine, but have documentation of a previous rabies vaccination, the vaccine is immediately boostered and the dog carefully observed for 45 days for any sign of illness.
For dogs that have never had a rabies vaccination, or don’t have documentation of a rabies vaccine ever being given, and have been exposed to a potentially rabid animal, the CDC and the American Veterinary Medical Association (AVMA) recommend immediate humane euthanasia. Unlike in humans, there is no post-exposure prophylactic treatment available for animals, and so the likelihood of the exposed dog developing rabies is fairly significant. Once the dog develops symptoms of rabies, he poses a significant risk of transmitting the virus to humans or other animals, which is why euthanasia before that happens is recommended. Another possible option for owners unwilling to euthanize but willing to take the responsibility is vaccination within 96 hours of the exposure followed by four to six months of strict quarantine. While in quarantine, the dog must be confined to an escape-proof enclosure and may not have any direct contact with humans or other animals. Each state defines the escape-proof enclosure differently; some states mandate quarantine in an animal hospital or animal control facility while others allow the dog to be quarantined at home in either a separate solid wall building with a roof, a cage or a pen, depending on the state. Any costs associated with the quarantine are the responsibility of the owner.
Once symptoms begin to occur, no treatment is available for dogs, humans, or other mammals. Humane euthanasia of animals is recommended at that point. In humans, supportive care is provided until death occurs. While it is technically possible for humans to survive rabies, the likelihood is extremely slim; only about 15 cases of humans surviving clinical rabies have ever been documented, and most of those that do survive have severe brain damage.
Prevention
Rabies in dogs is preventable using any one of the USDA-licensed canine rabies vaccines when administered according to the label. The rabies vaccine is administered to puppies at least 3 months of age, again one year later, and then every 3 years thereafter.
What does a vaccine do?
Normally when your dog’s body encounters a new virus or bacteria, the white blood cells of the immune system identify it as foreign, send out antibodies to destroy the invaders, and then remembers what the bacteria or virus looks like (its antigens). The first time your dog encounters a new germ, this process of identifying and destroying it takes several days – usually not soon enough to prevent illness, but the process helps stop the infection from becoming worse. The next time your dog encounters that same germ, his immune system remembers the germ and how to fight it, and so his immune response is much faster and much more robust, and your dog doesn’t become sick at all.
Vaccines help train the immune system to fight off an actual infection by introducing the germ to the body in a controlled fashion, in a way that won’t cause the disease. Then when the dog’s body encounters the actual germ, his immune system is already primed and ready to kill the invading germ. There are a few different ways to produce a vaccine; all licensed canine rabies vaccines in the United States are made with killed (inactivated) rabies virus.
The rabies vaccine is particularly important because the virus enters the nervous system and is out of reach of the immune system within a couple of days. This occurs before the virus is able to be killed off, and by the time the virus reappears in the saliva, it’s too late to save your dog. By vaccinating your dog against rabies, the immune system is already primed and begins attacking the rabies virus almost immediately and is able to remove the threat before the virus reaches the nervous system.
What are the benefits of vaccination?
The rabies vaccine prevents infection with an almost universally fatal disease. The vaccine not only prevents the disease in dogs, but is also an important component of keeping humans safe from rabies. Contact with unvaccinated rabid dogs accounts for approximately 99% of all human rabies cases worldwide, of which there are about 60,000 per year. There have been some recent developments in an oral vaccine that could be used in areas of the world with a large stray dog population, but until there is widespread vaccination of both owned and stray dogs worldwide, humans will continue to be at great risk of becoming infected with rabies from unvaccinated dogs. Thanks to widespread and continued canine rabies vaccination programs in the United States, the risk of dog to human transmission in the United States is virtually zero, but is still possible when unvaccinated dogs come in contact with wildlife.
As mentioned above, dogs with an unknown vaccination history or dogs that have never been vaccinated and come in contact with potentially rabid wildlife must be euthanized or else strictly quarantined for at least four months.
From a legal standpoint, a current vaccination against rabies is a requirement for dog ownership in all 50 states. A current vaccination status also provides protection for your dog should he bite someone. Some jurisdictions may require unvaccinated dogs to be surrendered for rabies testing so that if the person who was bit needs to begin rabies preventative treatment, it can be begun as soon as possible. The rabies test is performed on brain tissue which can only be obtained after the dog has been euthanized. With a current rabies vaccine, the biting dog needs only to be observed for 10 days and then declared to be healthy by a veterinarian at the end of the 10 days.
What are some of the concerns of vaccination?
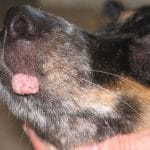
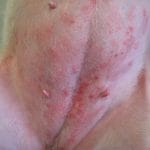
Some dogs do have an adverse reaction to vaccination. Most reported adverse reactions include a lump at the injection site, facial swelling, hives, vomiting, lethargy, generalized achiness, low-grade fever, and loss of appetite. Many of the adverse reactions are mild and will pass in a day or two, similar to how we might feel a little unwell for a day or two after receiving the flu vaccine. Other reactions that appear within 30 minutes of vaccination, including facial swelling, hives, difficulty breathing, and collapse are much more serious, as these are symptoms of an allergic/anaphylactic reaction. The reaction can be treated with an injection of steroids; veterinarians will often have dogs remain in the office for at least 20-30 minutes after vaccination just in case an allergic reaction manifests, particularly small breeds receiving a new vaccine. Unfortunately, death is also a risk with vaccines due to a severe anaphylactic reaction causing shock; 12 deaths were reported during the course of a three year period (2004-2007) in which 120 million vaccines were administered.
There is some concern that vaccines, and particularly the adjuvants used in those vaccines, can cause immune-mediated disease, specifically immune-mediated hemolytic anemia (IMHA) and immune-mediated thrombocytopenia (ITP). Adjuvants are substances added to a vaccine to boost the immune response and provide longer-lasting immunity. The issue has been studied extensively in millions of children, where an association was shown only with a specific MMR (mumps, measles, and rubella) vaccine on the order of one case of ITP per 21,000 to 40,000 vaccinations. However, the risk of developing ITP after recovering from measles is one in 3,000 to 6,000 cases. Similar studies have been performed in dogs, but with much smaller sample sizes (the largest study looked at 76 dogs), and only one suggested there might be a link while three others did not find a relationship. Mechanisms by which autoimmune diseases might be triggered by vaccines have been demonstrated, but studies that are well-controlled with a large sample size have not been performed, and so the evidence remains largely anecdotal.
How are adverse reactions handled?
If your dog has had an adverse reaction in the past, be sure to remind your veterinarian’s staff when scheduling your dog’s vaccine appointment. Depending on the severity of the reaction, your veterinarian will administer an injection of diphenhydramine (Benadryl) and/or a steroid about 15 minutes before administering the vaccine, and then may ask you and your dog to remain at the office for a short period of time after the vaccination for observation.
If your dog is due for several vaccines at once, they can often be given over the course of several weeks, one vaccine at a time. This keeps the immune system from being overwhelmed, and also helps isolate exactly which vaccine causes a reaction, if any.
You can consider running titer levels for some vaccines to see if your dog is still protected and therefore doesn’t need a booster. Unfortunately, this is not an option for the rabies vaccine due to state and local laws. Since a protective titer has not been established for the rabies vaccine (doing so would require deliberately exposing hundreds of dogs to a disease that is 100% fatal), regulations will not permit a titer in lieu of a current rabies vaccine.
Some states will allow rabies boosters to be skipped if a veterinarian is able to show that administering the rabies vaccine would be extremely detrimental to the health of your dog. A common example of this is if your dog is receiving chemotherapy, or has his immune system suppressed while recovering from an autoimmune disorder. However, your dog would then be considered to not have a current rabies vaccination, with all the legal ramifications of that situation, if your dog is exposed to rabies or bites a human or another animal, and so, very few states allow medical exemptions for the rabies vaccine. In those states that do allow the exemptions (usually only for a year), it is expected that your dog will be revaccinated once it is safe to do so.
Are we over-vaccinating for rabies?
One way the veterinary industry is trying to limit the number of adverse reactions is by reviewing how often vaccines need to be given in order to remain effective. The governing bodies of the veterinary profession have recently moved away from recommending yearly vaccinations for rabies (and distemper/parvo/adenovirus) and moved to a three year interval for those vaccines.
Earlier this year (2020), the Rabies Challenge Fund study was published. It attempted to show that dogs were still protected from the rabies virus five, six, or even eight years after the last rabies vaccination. Unfortunately, the study was flawed in many ways, such as not using the standard protocol of vaccinating at 12-16 weeks of age and again one year later; instead these dogs were vaccinated at 12 weeks and again 3 weeks later. When challenged with the rabies virus at five years after vaccination, they all survived, but so did most of the unvaccinated control dogs. Had the rabies virus been sufficiently active, all of the unvaccinated dogs should have died, so it’s impossible to draw the conclusion that the vaccinated dogs were still protected against rabies five years after their last vaccination. The vaccinated dogs were challenged again at six and a half years after their last vaccine and this time 20% (1 out of 5) of the vaccinated dogs died. When challenged again at eight years, 80% (4 out of 5) vaccinated dogs died. So despite their best efforts, the Rabies Challenge Fund was unable to show that extending the interval between rabies vaccinations beyond three years would still be protective. However, they were able to show (whether intentionally or not) that giving the rabies vaccine just once or twice does not confer lifelong immunity to rabies. Therefore, vaccinating every three years against this deadly disease is still the recommendation.
Take-away message about the rabies vaccine
While there is some risk with the rabies vaccine, the benefits far outweigh the risk. During the years 2004 to 2007, there were 8.3 reports of adverse reactions per 100,000 vaccines, or 0.0083%, and those reports ranged from swelling at the injection site, hives, vomiting, diarrhea, lethargy, mild fever, collapse, and yes, death. Given the public health risk associated with rabid animals – approximately 60,000 human deaths each year around the world, most of them children, and about 99% of the human cases were acquired from dogs – the rabies vaccine is not going to go away. Indeed, the rabies vaccine is a success story in the United States, with at least 6,900 confirmed rabid dogs in 1947 before vaccination became the law, and just 58 rabid dogs in 2016. There are ways to mitigate the risk by not giving multiple vaccines the same day or administering injectable Benadryl and/or steroids before the vaccine. Talk to your veterinarian about your concerns and how best to keep your dog protected while minimizing the risk of adverse reactions.



Will aggressive behavior after rabies shot ever go away? I want my sweet dog back!
I took my 6 lb 7 month old puppy in for her 1st rabies shot. Ever since that exact day, her behavior hasnt been her normal playful puppy self? She barks and growls at the wind meaning, for no reason at all. She’s stand offish. Not very affectionate. Sleeps more than usual. Seems aloof. Urinates more frequently, overreacts to sounds. I’ve given her CBD since she was 8 weeks old and she loves it. I just don’t understand her drastic change of behavior? I’m concerned and will be calling the vet tomorrow but wondered if anyone had any advice from similar experiences? She’s a pure bred min pin.
My 4 year old mini poodle, had the rabies/parvovirus-distemper combo/Bordetella. Three different injections, all in the neck. Four hours later, my dog was running around the house like crazy! Tossing pillows, pushing blanket off the bed and panting . I rushed her back to the vet, by then, the top of her nose into her eyes and ears was bright red. Swelling in her mouth area. Her temp was 105.5. They rushed her into the back and injected her in her back area with subcutaneous fluids with Benedryl and gave her Dexmethazone in her vein. We put ice cloths on her, and finally got her pretty much back to normal. I will not allow another vaccine without a titer., tho the rabies vaccine is probably the culprit. My breeder seems to think that if the shots were given to close together, it could cause a toxic reaction if they mixed.?? Anyone else have this experience?
Had a Grand Mal seizure after rabies shot he was 11 years old. Has not had one since and not on seizure medication
My Chihuahua was always a sweet lil guy sadly after a 2nd rabies vacs he had a bad reaction then noticeably he completely changed – even at a year after he’s aggressive towards my other dogs especially around food. He growls on the bed when they are not even near him it has truly broken my heart but I will continue to love him but I do discipline when the aggression begins to lesson his rage.