IN THIS POST
Key Takeaways
If you find a new bump on your dog’s lip that lasts more than two weeks, changes color, bleeds, or makes it hard for them to eat, it is time to see the vet. While many of these bumps turn out to be harmless, they can be much more serious in older dogs. A fine needle aspiration or biopsy is still the best way for us to know exactly what the bump is. Most causes are treatable, but oral melanoma is a life-threatening exception that needs a specialist’s help right away.
There are relatively few things that can cause bumps on the lips, snout, or chin of your dog. Most are benign and easily treatable, but bumps on an older dog’s lips are a cause for concern. This article covers the symptoms, causes, diagnostic tests, treatment, and prevention of bumps on your dog’s lips.
Not every bump looks the same. Some are pale pink or white and rough like a cauliflower. Others are red and irritated, or dark and flat. A few look completely innocent on the outside but are hiding something more serious underneath. Knowing what you are looking at makes all the difference.
Papilloma Virus (Warts)
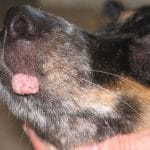
Dog warts are probably the most common reason a bump shows up on a dog’s lips or muzzle. They are caused by the canine papillomavirus (CPV), and more than 25 types of this virus have been identified in dogs. The classic presentation is a small, rough, cauliflower-like growth on the lips, inside the mouth, or around the muzzle. While the lips are the most common spot, these warts can occasionally pop up on the eyelids or even between the toes. They look unusual but are almost always benign.
Which Dogs Get Warts?
Mostly young dogs. Puppies and dogs under two years old are the most common victims because their immune systems are still figuring things out. Older dogs on steroids or chemotherapy can also pick up the virus since their defenses are similarly lowered. The virus spreads through direct contact with an infected dog or anything they have touched: toys, bowls, bedding. It needs a break in the skin to get in, so healthy intact skin is actually a decent barrier. Once exposed, it can take about 4 to 8 weeks before anything shows up.
How Are They Diagnosed?
When the cauliflower-shaped bump appears, it is pretty hard to mistake for anything else. Most vets can identify oral papillomas on sight. If something looks off, the growth is in an unusual spot, or it is not going away on its own, a biopsy is the next step to make sure nothing more serious is going on.
What Happens Next?
In most young, healthy dogs, nothing needs to be done. The immune system catches up and the warts disappear on their own within 1 to 5 months. If the bumps persist beyond three months, grow rapidly, or start interfering with eating, veterinarian evaluation is necessary. Possible treatments include surgery, cryotherapy, and others depending on the case.
Prevention is straightforward: keep infected dogs away from others until the warts are fully gone. For a deep dive into CPV, see Warts on Dogs: Symptoms, Causes, Treatment, and Prevention.
Malignant Melanoma
Oral melanoma is the most common malignant mouth tumor in dogs, and it is the one that warrants the most urgency. These tumors grow from melanocytes, which are the cells responsible for producing skin pigment. When those cells mutate malignantly, they can spread fast, traveling to the lymph nodes and lungs before the bump on the lip even looks serious.
What Does It Look Like?
The appearance of oral melanoma varies more than most people expect. Some tumors are dark and pigmented, sitting on the gums or lips like a bruised, raised mass. Others are completely pink or even white, flat and plaque-like, hiding on the inner surface of the lip or on the palate, which is the area at the top of the dog’s mouth. A pink bump on your dog’s lip is not automatically safer than a dark one. Melanomas without pigment, called amelanotic melanomas, are just as aggressive as the darker kind.
The tumor may look small on the surface. Underneath, it is often much larger, growing deep into the surrounding tissue and sometimes into the jawbone itself. Most dogs diagnosed with oral melanoma are over 10 years old.
The Symptoms: What to Watch For
- Bad breath that does not improve with dental care
- Drooling or saliva that is tinged with blood
- Panting
- Dropping food, reluctance to eat, or difficulty chewing
- Swelling on one side of the face
- Loose or missing teeth near the growth
- Reluctance to be touched on the head
- Swollen lymph nodes under the jaw or in the neck
Which Breeds Are at Higher Risk?
Genetics plays a significant role in this type of cancer. Chow Chows, Schnauzers, Cocker Spaniels, Golden Retrievers, Gordon Setters, and Miniature Poodles are all breeds with a documented higher risk for oral melanoma. If your dog is one of these breeds and is over seven years old, a quick look inside the mouth during every vet visit is worth asking for.
Diagnosis and Staging
A biopsy is the only way to confirm melanoma and understand how it is likely to behave. A fine needle aspirate can give some early information but often misses what the pathologist needs for a definitive answer. Once the diagnosis is confirmed, staging begins: chest X-rays, lymph node sampling, and sometimes an abdominal ultrasound to find out whether the cancer has already metastasized, or spread to other parts of the body.
Staging directly determines prognosis. The prognosis is reported as a median survival time (MST), which represents the length of time at which half the dogs at that stage of cancer have died and half are still alive. The table below shows approximate survival times based on historical data from surgery-only cases. These numbers are not a sentence; they are a starting point for a conversation with a veterinary oncologist.
Stage I
Tumor: Less than 3/4 inch, no spread
Treatment: Surgery alone
Median Survival: 15 to 18 months
Stage II
Tumor: 3/4 inch or larger, no spread
Treatment: Surgery with or without radiation
Median Survival: Approximately 6 months
Stage III
Tumor: Larger than 1.5 inches or lymph node spread
Treatment: Surgery, radiation, and ONCEPT
Median Survival: 3 to 4 months
Stage IV
Tumor: Spread to lungs
Treatment: Palliative; chemotherapy may help
Median Survival: 1 to 2 months
A Personal Note…
It is easy to look at these median survival times and feel defeated, but these figures are often based on the most conservative historical data, cases involving surgeries alone. In actuality, outliers are not uncommon. They are pets who outlive these averages through a combination of treatment, lifestyle changes and diet. These numbers are a starting point for planning, not a predetermined timeline for your pet.
Chloe was diagnosed with Urothelial Carcinoma (UC), also known as Transitional Cell Carcinoma (TCC) or bladder cancer, and the internist told me she had 2 to 3 more months to live. She went on to live for another year. Of course, every dog is different, every cancer is different, and every case is unique. But I wanted to share this so that pet parents understand that these numbers are not set in stone. I have seen more than a handful of stories in the dog cancer groups I belonged to where dogs outlived their prognosis.
— Chloe’s Mom, Content Director, DogsCatsPets.org
Treatment: What Are the Options?
Surgery
Surgical removal of the tumor is the standard treatment for melanoma. The goal is to remove as much of the tumor as possible; any tumor cells left behind will eventually regrow. When the tumor has infiltrated the jaw bone, removal of the affected jaw is necessary to remove the entire mass. Dogs adapt to this better than most owners expect, and quality of life after jaw surgery is generally good.
Radiation Therapy
If surgery is not an option due to the location of the tumor, or if surgery is not able to completely remove the tumor, radiation therapy is an option.
Radiation therapy uses high-energy beams to target and destroy cancer cells that surgery could not reach. In dogs with oral melanoma, it is typically delivered in a series of sessions under general anesthesia, since the dog must stay completely still.
The number of sessions varies depending on the protocol, but melanoma responds relatively well to radiation compared to some other cancers. About 70% of dogs treated with combined surgery and radiation are free of disease at the primary site one year later. That is a meaningful number worth discussing with a specialist.
The ONCEPT Vaccine
ONCEPT is not a first-line treatment. It is given after local disease control has been achieved through surgery or radiation. It is the first licensed therapeutic vaccine for cancer in either dogs or humans, and it is available at specialty veterinary oncology practices in the United States. It was conditionally licensed by the USDA in 2007 and received full approval in 2010.
The vaccine introduces a human version of a protein found on melanoma cells. Because it is human rather than canine, the dog’s immune system flags it as foreign and mounts a response. In doing so, it also targets the dog’s own melanoma cells. It is essentially teaching the immune system to recognize the cancer cells as a threat.
Does it work? The data is mixed. A large review of 131 dogs treated with ONCEPT reported a median survival of 510 days. Several other retrospective studies found no significant difference compared to dogs that did not receive the vaccine. It was not tested in randomized clinical trials, which is the standard the FDA requires for drug approval in humans. The USDA, which governs veterinary biologics, operates under a different and less stringent approval process than the FDA. That is how ONCEPT reached approval despite the lack of randomized trials. If your dog is a candidate for the vaccine, the conversation is worth having with a veterinary oncologist.
Chemotherapy
Chemotherapy is usually the last resort since melanoma tends not to respond well to it. It may help once the disease has spread to other parts of the body, such as in stage IV disease.
One study using a combination of carboplatin, a platinum-based chemotherapy drug that works by interfering with cancer cell DNA replication, and the anti-inflammatory drug piroxicam increased median survival from 30 days to 119 days in advanced cases. However, it did not show a significant benefit for earlier stages.
Your veterinarian will determine the appropriate medication and dose based on your dog’s breed, weight, and specific condition.
Squamous Cell Carcinoma (SCC)
Squamous cell carcinoma, or SCC, is the second most common malignant oral tumor in dogs after melanoma. It grows from the cells that line the gums and inner mouth surfaces, and it has an unfortunate habit of invading the jawbone before it even looks that big from the outside.
The good news compared to melanoma: most forms of SCC are slower to metastasize to distant organs, which gives treatment a better chance of working.
What Does It Look Like?
SCC usually shows up as a pink or red mass on the gumline that bleeds easily when touched. It can also appear as a raised, irregular lump or a thickened, white or red plaque that looks almost like inflamed gum tissue. Early cases are frequently mistaken for severe gum disease, which is one reason they get caught late.
Like melanoma, the visible part is often just the tip of the iceberg. The tumor extends deep into the tissue and bone underneath, much farther than the surface suggests. Any red or pink growth on the gumline that does not improve after a dental cleaning needs a biopsy, not more brushing.
The Symptoms: What to Watch For
The clinical signs of SCC overlap heavily with melanoma, which is exactly why a biopsy is the only reliable way to tell them apart.
Watch for:
- Persistent bad breath
- Oral bleeding
- Loose teeth
- Facial swelling
- Drooling
- Visible discomfort when eating
If your dog is suddenly dropping food or chewing on one side only, a same-week vet visit is needed.
Diagnosis
A biopsy with full pathology review is required for diagnosis. The vet will typically recommend an anesthetized oral exam first, since a thorough look inside the mouth is not really possible in an awake dog. Dental X-rays and CT imaging show how far the tumor has grown into the bone, which directly affects what surgery is possible.
Treatment and Prognosis
Surgery
Surgery with wide margins is the standard treatment for non-tonsillar SCC (SCC that originates on the gums or inner mouth, not in the tonsils at the back of the throat). If the jawbone is involved, removing part of the jaw is often necessary to get clean margins, meaning no cancer cells were found at the edges of the removed tissue.
Dogs handle this surgery well in most cases and quality of life after recovery is generally good.
Radiation
Radiation is used when surgery is not an option or when margins are incomplete. SCC does not respond well to chemotherapy on its own. For non-tonsillar SCC caught early and treated aggressively, some studies report median survival times over 15 months and one-year survival rates above 80%, which is considerably better than oral melanoma.
A Note on Tonsillar SCC
Tonsillar SCC is a different story: it spreads to the lymph nodes in more than 70% of cases at diagnosis and carries a much worse prognosis. If the tumor originates in or near the tonsils, staging and specialist referral are even more urgent.
Your veterinarian will determine the appropriate treatment plan based on tumor location, size, and stage.
Canine Acne
Dogs can get acne. It shows up as red bumps, blackheads, or whiteheads on the chin, lips, and muzzle, and it has nothing to do with hormones the way human acne does.
In dogs, it usually starts with trauma to the hair follicles. The follicle ruptures, the contents spill out, and the surrounding skin gets irritated and inflamed. Once the follicle ruptures and the skin is compromised, an infection can develop on top of the inflammation.
Which Breeds Are Most Affected?
Short-coated breeds seem to be affected the most, and genetics definitely plays a role. Boxers, English Bulldogs, Great Danes, German Shorthaired Pointers, Doberman Pinschers, Rottweilers, Mastiffs, and Weimaraners all show up more often in the exam room with this condition. Occasionally food or environmental allergies can be culprits too.
What Does It Look Like and How Is It Diagnosed?
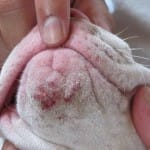
The classic presentation is a cluster of small red bumps, blackheads, or whiteheads on the chin. Severe cases can progress to swelling of the whole muzzle with open sores and scabbing.
A vet can usually diagnose this on sight, but a skin scraping may be done to rule out mange. A skin swab, or cytology, can check for bacterial infection if the lesions look infected.
Treatment:
Topical veterinary-grade benzoyl peroxide is the go-to treatment. It flushes out the hair follicles and keeps bacteria in check. For infected cases, steroids or antibiotics may be added.
Your veterinarian will determine the appropriate medication and dose based on your dog’s breed, weight, and specific condition.
Home Care:
A few simple changes at home can make a real difference:
- Do not squeeze or pop the acne. It feels satisfying but it makes things worse by rupturing more follicles.
- Switch to stainless steel or ceramic bowls. Plastic bowls scratch easily, harbor bacteria, and create repeated friction trauma on the chin during meals.
- Wipe your dog’s muzzle clean and dry after every meal. For dogs with deep facial folds, those folds need daily cleaning too.
- Look for the source of the trauma. Rough bowl edges, rooting in dirt, and face scratching are common triggers worth addressing.
For a deep dive into canine acne, see Dog Pimples – Causes, Treatment, and Pictures.
Lip Fold Dermatitis
Lip fold dermatitis doesn’t usually cause distinct bumps on a dog’s lips, but instead causes redness, irritation, swelling, alopecia (hair loss), and discomfort. This condition is less about bumps and more about what is happening inside the skin folds of the lower lip.
In breeds with long, droopy upper lips, like Saint Bernards, Spaniels, English Bulldogs, and Basset Hounds, the upper lips trap moisture from the mouth against the lower lips, resulting in a perfect environment for overgrowth of the normal skin bacteria and yeast. The microbes produce toxins and breakdown products that cause irritation, inflammation, and breaks in the upper skin layer, leading to further penetration of the microbes into the skin, causing chronic infection and inflammation.
Dogs with poor dental hygiene tend to have it worse. Bacteria from gum disease drains right into those folds and adds to the problem. The giveaway is usually the smell: a sour, musty odor that no amount of teeth brushing seems to fix.
Diagnosis:
Diagnosis of lip fold dermatitis can usually be made based on clinical signs alone. The redness and irritation do not generally extend beyond the area of folded skin. To confirm, the vet may perform a skin cytology, which involves running a moist cotton swab along the area of irritation and into the skin fold, then rolling the swab onto a microscope slide.
The result will reveal whether it is a bacterial infection, a yeast infection, or both, which determines the treatment.
Treatment and Prevention:
Treatment of lip fold dermatitis starts with clipping any hair in the area, so that the hair does not continue to trap moisture and microbes. The lip folds will need to be cleaned once or twice daily to remove any debris and microbial overgrowths. Clean the fold once or twice a day with antiseptic wipes containing chlorhexidine or ketoconazole, both of which target the bacteria and yeast causing the problem.
A pet-safe barrier cream such as Zymox Topical Cream or plain petroleum jelly can help keep the area dry between cleanings. Always confirm with your veterinarian before applying any product to an open or irritated fold.
Safety Warning
Never use human diaper rash creams containing zinc oxide on dog skin. Dogs lick their lips constantly, and zinc oxide is toxic when ingested. Use only zinc-free, veterinarian-approved barrier products.
In severe and/or chronic cases, cheiloplasty, a surgical procedure performed under general anesthesia to remove the lip fold permanently, is the most effective long-term solution.
Frequently Asked Questions
Can my dog get warts from me, or can I get them from my dog?
No. Canine papillomaviruses are entirely species-specific. Humans cannot contract warts from dogs, and dogs cannot acquire them from people or other animals.
Is a pink bump on the lip less dangerous than a dark one?
Not necessarily. While melanomas are often pigmented, amelanotic melanomas are pink and carry an equally poor prognosis. Any new growth on a dog’s lip, regardless of color, requires professional evaluation.
How do I tell the difference between a pimple and a tumor on my dog’s chin?
Canine acne typically presents as multiple small red bumps or blackheads clustered on the chin. A tumor is usually a single, distinct, enlarging mass. If a bump does not resolve within two to three weeks, grows in size, bleeds, or changes in appearance, a veterinarian should take a look.
What causes bumps on a dog’s snout or around the muzzle?
The most common causes are viral papillomas, canine acne, and lip fold dermatitis. In older dogs, squamous cell carcinoma and melanoma must also be considered. The dog’s age, breed, and the appearance of the lesion help narrow the differential.
How can dog lip bumps be prevented?
Prevention depends on the cause. For lip fold dermatitis, maintain excellent oral hygiene and clean the skin folds daily. For canine acne, switch to stainless steel or ceramic bowls and wipe the muzzle dry after meals. For viral papillomas, limit contact between young or immunocompromised dogs and dogs with visible warts. For melanoma and SCC, early detection is the best tool: inspect the lips and gums weekly and schedule regular veterinary oral exams, especially for dogs over seven years old.
When to See a Veterinarian
Most bumps on a dog’s lips turn out to be nothing serious. Warts in young dogs go away on their own. Acne and lip fold dermatitis clear up with the right topical routine. But oral melanoma and squamous cell carcinoma are aggressive cancers that look completely innocent in the early stages, and early detection genuinely changes outcomes.
A good rule to follow: any bump that has not started to change or shrink within two to three weeks, or any growth that is bleeding, changing color, or appearing in a dog over seven years old, deserves a vet visit. Do not wait to see if it gets better. A fine needle aspirate takes about five minutes and gives a first answer without surgery.
When in doubt, get it checked. That is always the right call.
Note from the Editors: This guide was originally authored by Dr. Winnie, DVM. It was updated to reflect current veterinary safety standards. To ensure the highest clinical standards, this post is currently in our queue for a veterinary re-review.
References
- PubMed / PMC: The Use of Oncept Melanoma Vaccine in Veterinary Patients: A Review of the Literature
- PubMed: Use of Oncept melanoma vaccine in 69 canine oral malignant melanomas in the UK
- PubMed: Multimodality treatment including ONCEPT for canine oral melanoma: A retrospective analysis of 131 dogs
- Boehringer Ingelheim Animal Health: ONCEPT Canine Melanoma Vaccine, DNA: Product Information
- PubMed: Papillomavirus: Clinical Presentations and Treatment Approaches
- PetMD: Warts in Dogs
- PMC: A retrospective review of outcome and survival following surgery and adjuvant xenogeneic DNA vaccination in 32 dogs with oral malignant melanoma
- Cornell University College of Veterinary Medicine: Oral Squamous Cell Carcinoma in Dogs
- VCA Animal Hospitals: Oral Tumors: Squamous Cell Carcinoma
- dvm360: Finding and treating oral melanoma, squamous cell carcinoma, and fibrosarcoma in dogs
- Merck Veterinary Manual: Oral Tumors in Small Animals
- NC State College of Veterinary Medicine: Canine Oral Melanoma